|
Inspiration, news and knowledge from Polio Experience Network |

Standing With Confidence
by Elinor Young
The Way We Do It
Eaves-droppings by Mouse In Corner
P.O.S. Library
An interview with Helen Gress
by Sharman Collins
Post-Polio Protein Power: Eat Well, Be Well
by Dr. Bruno
Our Offer
Copyright information
from Sharman Collins
Happy Holidays from my house to your house!
After a short summer but a beautiful fall, I hope you are ready to curl up by the fireplace and keep warm.
I hope to spend time this winter rocking my baby granddaughters, Courtney Lauren and Madelaine Elise. And play in the snow with my grandson, Kenneth Thomas. I am happily anticipating shopping for toys this Christmas.
On November 23, Jeanann Eckert, AC, will be our speaker. Jeanann is a licensed practitioner of Traditional Chinese Medicine and has been in practice since 1985. She taught in San Diego at the Pacific College of Oriental Medicine for eight years. She also has a background in Respiratory Therapy. Jeanann has resided in Spokane with her daughter for four years. She practices in two offices–one on the north side and one on the south hill. This will be an informative meeting. I know you are all interested in hearing how acupuncture could help post-polio survivors cope with symptoms.
On January 25, 2000, our meeting will be a discussion group utilizing the expertise of our local group members. Sharing coping skills helps us all deal with the adjustments that need to be made in order to function with post-polio syndrome.
Steve Whitley, formerly associated with R & S Wheelchair, now working with Choice Medical Supply, will come to our meeting on February 22 to be our speaker. He will attend a national conference in January dealing with aids for independent living. Steve is excited to show us all the new equipment that is available.
As you can see, we have great meetings planned to close out the year and to welcome the New Year! I am looking forward to seeing you at Shriners Hospital, W. 911 5th Avenue, at 6:00 p.m. There is easy access from the free parking garage located under the hospital. If you are able to join us for dinner in the 4th floor cafeteria, please be there by 5:00 p.m.
Much love from your friend,
Sharman

“She was the first polio patient of 1952 at St. Luke’s hospital in Spokane,” Mr. Carper said. I hadn’t known that. I knew that I was hospitalized in January, but didn’t know I had that special distinction until Mr. Carper mentioned it when he came to speak to our Polio Outreach of Spokane meeting.* He was the physical therapist at St. Luke’s hospital in 1952. I was just five years old, but I have clear memories of snow falling as my dad tried to walk quickly yet carefully as he carried me up the sidewalk to the hospital’s emergency entrance.
“Hurry, Daddy. I can’t breathe.”
The next thing I remember was waking up in the white world of isolation curtains. A pull-string to call a nurse was pinned to the bed near my head, but my arms wouldn’t move to reach and pull it. I couldn’t move anything but my eyes, as they took in the strangeness of it all.
Mr. Carper also told another story I hadn’t remembered: “Elinor was crawling on the exercise mat,” he said, “and I told her, ‘You look like a snake, crawling like that.’ ‘I do not!’ she countered. ‘Yes you do.’ ‘No I don’t! Snakes don’t crawl with arms and legs.’ ‘How do they crawl, then?’
After some contemplation, Elinor replied, ‘They crawl with their all-together. Except their eyes.’”
Hearing that story made me smile because it and my own memories of those hospital days, as I reflect upon them, show me a little girl who had a confident self-identity. An identity that stayed intact while growing up visibly different from children who could run, jump, ride a bike, walk without a “galumph,” bat a baseball and carry their own books to school.
As I rub shoulders with other polio survivors in our support group or on the Internet, I see that not all of us came through this devastating disease with such confidence — and no wonder. Some of us were teased unmercifully at school or shunned by people who didn’t know how to react to someone who is nonstandard.
So what gave me the confidence of a positive personhood? By what power could I refuse to internalize society’s insults, rebuffs and mis-descriptions of me? I believe the answer to that has it’s groundings in those same early months in the hospital after getting polio.
My daddy, like the father of any five-year old girl from a happy home, was my protector and the one who made bad things all better again. Then polio struck and daddy couldn’t be there in the hospital to help and protect. He couldn’t be there when I was all alone and frightened, feeling life slip away. He couldn’t help when my lungs finally lost the strength to pump air any more.
My daddy wasn’t there, but he had taught me that God was always with me, would never leave me, and could help when no one else could. So, almost like an automatic reflex, that night when I was so frightened that my life was ending, with child-like simplicity I asked God to please help. He did. Immediately I felt peace and knew he was there, making sure I was O.K. At that moment I knew that I mattered to God; I was important to him. He had a plan for me, he loved me and he would see me through, no matter what. He became my other, unlimited “Daddy.”
I suppose that can be seen as pretty incredible insight for a five-year old. When you look at it, though, it’s actually quite simple. And there in the hospital, as “the Sunday School lady” came every week to each room with her flannel graph board and told Bible stories 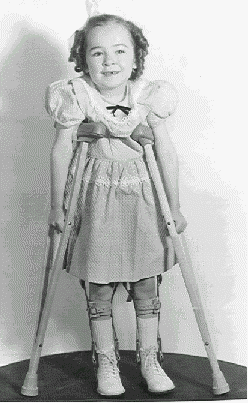 about Jesus, my trust in his love and my knowledge of his smile on me became firmly anchored in his own words.
about Jesus, my trust in his love and my knowledge of his smile on me became firmly anchored in his own words.
So, by the time I left the hospital, I was standing confidently, not only on the outside but on the inside as well. My identity was firmly rooted in God’s statement of his love for me, and nothing has or ever can shake that.
“Who shall separate us from the love of Christ? Shall trouble or hardship ….? No, in all these things we are more than conquerors through him who loved us.”
Romans 8:35-39 ____________________
If you want to discuss the concept of this article with Elinor, she would be happy to hear from you.
________________________
*See the “Eaves-droppings” column in this issue.
This photo is of 6 Yr. old Elinor Young and was given to her by Emery Carper
the night he spoke at the Polio Outreach of Spokane meeting.
 The Way We Do It
The Way We Do It
How can we reduce the aches and pains connected with the way we have to use our bodies, or how can we avoid some of the pain to begin with? These ideas were gleaned from friends who passed them on to email lists: From: Mike Drummond
To: post-polio@egroups.com
Hi, gang. Today I have started using a remote keyboard and mouse on my office computer. I am able to sit far enough back from the screen to prop my feet on the computer desk and work with the keyboard in my lap. I can use the mouse and keyboard anywhere I want to without worrying with cables. My hands have not quite gotten accustomed to this keyboard, but before the day is over, I’ll be OK. It really helps to get my feet up for awhile. I bought a Logitech kit for $99. [Later Mike wrote, “As a follow up to the original message, now that I have used the remote mouse and keyboard for several weeks, it is really helpful and reduces muscle strain.”] — Carlton M. (Mike) Drummond Director of Academic Computing, Mercer University
——————-
From: Hilary Hallam
To: post-polio@egroups.com
ERgonomic keyboard is great. Took away a lot of pain from my arms. Has the tab and backspace key in the middle as well, and it only took 2 days to get used to it. Now I can barely type on straight one. But having wrists in line with shoulders is certainly an advantage, eliminated most of my wrist pain and can type for longer. Palm rest in front helps as well can put hands on front and type…… but I do stop every few lines and rest just for a few seconds… dont keep repeating movements too often. Pace and rest them.… hils. — Hilary Hallam (Hon Sec) ICQ 2299824 Lincolnshire Post-Polio Network: http://www.zynet.co.uk/ott/polio/lincolnshire
——————-
From: Margaret Lockhart To: POST-POLIO-MED@MAELSTROM.STJOHNS.EDU I have a long tube sock that I filled with rice and tied. I put it in the micro-wave for 3 or 4 minutes and then sit with it around my neck. It stays hot a very long time and really helps my neck pain!!
–Margy

Overheard at Polio Outreach of Spokane…
POS’s August meeting (which by now seems a long time ago, but you know how printing deadlines are…) was so interesting!
The featured speaker that night was Mr. Emery Carper, P.T. Mr. Carper was the physical therapist at St. Luke’s Hospital in Spokane beginning in 1951. At that time physical therapy was unknown to most of the general public, but much in demand by hospitals involved with treating polio victims. In fact, when Mr. Carper began his PT practice, “physical therapy” was almost synonymous with “polio rehabilitation.”
“St. Luke’s Hospital was the main polio hospital for eastern Washington then,” he said, “and full of polio patients.” There were so few therapists available for hire that he was able to name his price. A whopping $325 a month!
Though now retired, Mr. Carper has kept in contact with some of his patients through the years. In fact, five of them were in the meeting that night. Pretty amazing!
Mr. Carper related some poignant stories of some of the polio patients he treated in those early days. “To exercise people in iron lungs, I had to put my arms in special sealed holes and try to move their limbs for them. It was very difficult,” he said.
With tears Mr. Carper told of a malnourished little boy from an abusive home who was even more unwanted when he got polio. “We (the hospital staff) kept him two months beyond what we should have so that he could have nutritious food and kindness a little longer. He didn’t want to go home.”
Mr. Carper also talked about a young mother who had polio. “My wife and I had the wonderful privilege of taking care of that patient’s little girl while the mother was in Boise for several weeks of rehab,” he said.
“During those late epidemic years it was estimated that for every polio patient in the hospital, there were 100 who had light cases and were not hospitalized,” Mr. Carper told the group. “I read later a figure of 200 for every person hospitalized,” he added.
“You will remember the stories about the bad batch of polio vaccine from the Cutter laboratory,” Mr. Carper continued, “The polio that people got from that was awful. Unlike most other polio patients, they never were able to regain anything after their initial paralyzation. It was just awful.”
A technique Mr. Carper learned in the middle of his career was Shiatzu. He lamented that he did not know this method of therapy during the years of the polio epidemics. “It probably would have helped many of my polio patients, and may still be of help to those who have access to it,” he said.
Mr. Carper brought with him various handouts, including ones dealing with Shiatzu. Darlene got a copy of everything for the library and for anyone who wants one. You can find her address in the library box below. And I promise – I won’t get any copies to tear up for a bed in my mouse hole. Sounds comfy, though….
Interview with Helen Gress
By Sharman Collins
I spent a delightful hour with Helen talking about the events that have shaped her life. Our conversation was punctuated with laughter. If you need to be cheered up, call Helen!
Helen was born in Spokane at Deaconess Hospital on August 27, 1928. She was one month premature. “I started out in a hurry and I have been trying to catch up ever since.” Her childhood was spent living with various relatives in Washington, Oregon, and California.
Married on February 9, 1947, Helen and her husband had six children. In 1957 while she was living in Yakima, Helen contracted polio. She was in the hospital for ten days and was treated for non-paralytic polio.
Helen worked hard at whatever she did. She spent many years working as a waitress in Chattaroy and also in Spokane. And she started her own business –Helen’s As New Shop–a clothing consignment store.
Helen began to experience muscle weakening of her hands and arms in 1975. Her malady had no name and physicians told her that her symptoms were “all in her head.” Plagued with muscle weakness, pain and fatigue, Helen had to quit working in 1980. She was finally diagnosed with post-polio syndrome by Dr. Vivian Moise in 1990.
In addition to polio-related problems, Helen has been totally blind since 1993. When she was suffering from allergy problems in 1976, her physician prescribed cortisone drops for her eyes. Over the years she also had been given many cortisone shots for bursitis in her joints. She developed cataracts as a result of this over-dosage of cortisone. Surgery was not able to correct the damage and she was declared totally blind in 1993.
Helen receives help from the COPES program. She fell and injured her back in September and was in Deaconess Hospital and St. Lukes Rehabilitation Hospital for several weeks. She has an aid come to her home several hours a day to help her. It’s not enough help, and soon Helen will need to make other arrangements.
Helen attended some of the first meetings of our support group. She heard about our group in 1991 when she met a women on the bus who also had post-polio syndrome. Helen’s family is spread around Washington, Oregon, and Hawaii. She now has 13 grandchildren and 6 great-grandchildren. Her walls are covered with pictures of her family and she will proudly tell you about them.
I asked Helen what she does to keep busy. She listens to books on tape. Very knowledgeable about supplements and a healthy diet, Helen has become an expert at maintaining her health at the best level possible. I asked Helen how she manages to stay cheerful in the face of so much adversity. Without hesitation, she replied that her faith in God is what keeps her going. She no longer holds onto the anger that once made her bitter when she lost her eyesight. “The Lord keeps us here as long as he has a job for us to do.”
Helen’s “job to do” was obvious. She is an example to me of how someone firmly grounded in her faith in God can rise above the circumstances of her daily life.
“…….but those who hope in the Lord will renew their strength. They will soar on wings like eagles; they will run and not grow weary, they will walk and not be faint.” (Isaiah 40:31)
Post-Polio Protein Power: Eat Well, Be Well
Dr. Richard L. Bruno
 “Breakfast? Sorry, don’t have the time. In the morning there’s too much to do, like showering and dressing and getting to work. I grab a cup of coffee (or two or three) and maybe a donut at work…”
“Breakfast? Sorry, don’t have the time. In the morning there’s too much to do, like showering and dressing and getting to work. I grab a cup of coffee (or two or three) and maybe a donut at work…”
“Lunch? Don’t think so. I’m still catching up from my late start in morning. I grab a cup of coffee (or two or three) and maybe wolf down half a Big Mac…”
“Dinner? I’m either too tired or hungry as Patton’s Third Army. I either defrost a piece of pizza and drag myself into bed or eat everything that isn’t nailed down!”
“So why am I totally exhausted but can’t stop gaining weight?”
Americans are not very good at taking care of themselves. American’s with disabilities are no better, and maybe a little worse, at self-care because it takes so much time to do things non-disabled folk do in a flash, like showering and dressing. There’s hardly any time or energy left for planning meals, shopping, cooking … or even eating.
However, people with disabilities pay a higher price for lack of self-care than do people without disabilities. For those who use wheelchairs good eating habits and proper nutrition are essential, not only for general good health, but also to prevent bowel and urinary problems, to prevent weight gain, and to maintain a decent level of energy.
Polio Survivors vs. Breakfast.
One group of people with disabilities shows the consequences of poor eating habits: North America’s 1.8 million polio survivors. Nearly 76 percent of polio survivors experience Post-Polio Sequelae (PPS), the often disabling symptoms — fatigue, muscle weakness, joint and muscle pain, cold intolerance, and difficulty sleeping swallowing, breathing — that occur about 40 years after their original bout with polio.
PPS requires polio survivors to use new assistive devices or aids they discarded years ago, like braces, canes, crutches, wheelchairs and scooters, to slow down and to rest during the day. The problem is, polio survivors are Type A, hard working, pressured, perfectionist super-achievers who have pushed themselves beyond their physical limits and allow no time for self-indulgent luxuries — like food.
Polio survivors don’t want to slow down or rest, not only because they’re afraid if they are less Type A people won’t like them, but also because they are afraid of gaining weight if they become more sedentary. But they shouldn’t be afraid. Food is good! Eating properly doesn’t lead to becoming fat, it actually reduces PPS symptoms.
Dr. Susan Creange at the Post-Polio Institute discovered that polio survivors with blood sugar levels in the low normal range have as much difficulty paying attention and concentrating as would diabetics with blood sugars as low as if they had taken too much insulin.
“Polio survivors’ ‘Type A diet’ — three cups of coffee for breakfast, skipping lunch and eating pizza for dinner — is actually starving their nervous systems’ and causing PPS symptoms,” says Creange. The relationship between diet and PPS was seen in the 1998 National Post-Polio Survey: the less protein polio survivors had at breakfast the more severe were their daily weakness and fatigue.
Why do polio survivors function as if they have low blood sugar and report more symptoms when they don’t eat protein at breakfast? Because polio survivors are running their nervous systems on “half a tank of gas.” About 50 percent of all brain stem and motor neurons were killed decades ago by the polio virus. What’s worse, the metabolic apparatus, the internal power plant, of the neurons that survived the original polio virus infection was severely damaged.
So polio survivors have been running their full-tilt, Type A lives on half the normal number of neurons, neurons that are less able to use their only source of fuel, blood sugar. Dr. Creange found that even normal levels of blood sugar were not enough to fuel the remaining polio virus-damaged, metabolically impaired neurons. That’s where protein at breakfast comes in.
Protein: The fuel that keeps on giving.
Protein provides a long lasting, “slow-release” supply of blood sugar throughout the day. Polio survivors who had protein for breakfast reported less PPS symptoms because their fuel tank stayed full longer. They didn’t need to “fill up” throughout the day with short-lasting sugar fixes, like soda or candy bars.
When we ask our post-polio patients to eat protein every day at breakfast, and have small, non-carbohydrate snacks throughout the day, they report an almost immediate reduction in nearly all the symptoms of PPS, especially fatigue. But “protein power” diet is neither a fad nor a miracle: it’s just common sense. No engine can be expected to run without gas.
 And having protein at breakfast isn’t good only for polio survivors. Mom was right: breakfast is the most important meal of the day for everyone, but especially for people with damaged or compromised nervous systems. Folk with MS (for whom low energy and fatigue can be disabling) those with ALS and Guillian-Barre Syndrome need to feed their damaged neurons first thing in the morning.
And having protein at breakfast isn’t good only for polio survivors. Mom was right: breakfast is the most important meal of the day for everyone, but especially for people with damaged or compromised nervous systems. Folk with MS (for whom low energy and fatigue can be disabling) those with ALS and Guillian-Barre Syndrome need to feed their damaged neurons first thing in the morning.
Those with spinal cord injuries, CP and spina bifida, who use more energy just getting showered and dressed than does a non-disabled person who runs a mile, also need protein early and often. It’s a good idea to eat breakfast before showering to “break your fast” and fill your tank before your neurons need the fuel.
Our patients worry that using a wheelchair, resting more and having breakfast will cause them to get fat and have more PPS symptoms. A four-year follow-up study found that U.S. and Swedish polio survivors, living their typical “use it or loose it” lifestyles without using new assistive devices or resting, lost equal amounts of leg muscle strength, about 2 percent per year. However, when subjects from the two countries were looked at separately, the Swedes gained only 6 ounces per year, while the Americans gained over 2 pounds; that’s 220 percent more weight!
Although weight gain alone is not responsible for the progression of muscle weakness in polio survivors, it is Americans’ high fat, Big Mac diet that causes them to get fat. You can fuel your neurons, feel stronger and less fatigued without gaining weight, if you choose low fat, low cholesterol sources of protein. In fact many of our patients, even as they slow down, sit down more, and use a scooter, lose weight (about a pound per week) if they eat more protein, reduce portion size and limit carbohydrates.
We aren’t recommending one of those “all protein, no carbohydrate” diets. We aren’t recommending a “diet” at all, but a method for eating healthy every day. We suggest 16 grams of protein at breakfast; that’s about 1/4 of the daily protein requirement (70 grams) for a 150-pound person. (Always check with your doctor, especially if you have kidney problems, before changing your diet and ask to have your cholesterol measured at your yearly check up.)
Look at the list of protein-rich foods and select different breakfasts so you can have a variety throughout the week. Remember, you want foods that have more grams of protein than they do fat.
________________________________
Dr. Richard Bruno is director of the Post-Polio Institute, Englewood (NJ) Hospital and Medical Center, and Chairperson of the International Post-Polio Task Force, 201-894-3724, toll free: 1-877-POST-POLIO or e-mail c/o PPSENG@AOL.COM. Retrieved September 17, 1999 from http://members.aol.com/harvestctr/Library/prodiet/l. Used by permission.
Polio Outreach of Spokane Library
Your resource for information on post-polio syndrome and disability issues.

LIBRARY REPORT:
Here are the titles of the articles Emery Carper left with our group. They are now available to you.
- The Healing Touch from Japan: Spokane therapist uses acupressure (newspaper clip)
- The Human Touch: Therapist Emery Carper is a firm believer that technology will never replace skilled hands (newspaper article)
- Handout of acupressure points
We have other articles and books about acupressure, acupuncture, and massage therapy. Borrow and compare!
Our Offer:
If you want to receive PEN & ink by normal mail, send a request with your mailing address to:
P.E.N. S. 508 Shoreline Drive
Liberty Lake, WA 99019
We would appreciate a donation for printing and mailing costs, if you are able to do that. If you want to a subscription, let us know.

